The April 2010 edition of the Journal of Periodontology had an article entitled “Tissue Biotype and Its Relation to the Underlying Bone Morphology”, authored by Jia-Hi Fu et al. In the article, Cliffy’s and Shanley’s tissue biotype definitions are referred to. They define thin tissue as having a gingival thickness of <1.5 mm, and thick tissue as having a thickness of ≥ 2mm. In Jia-Haifa’s study, the mean buccal soft tissue and bone thickness of the maxillary anterior teeth at 2mm below the bone crest were respectively .5mm +/- .24mm and .83mm +/- .32mm. These results are in agreement with previous studies.
Tissue Biotypes
It is important to consider the tissue biotype before the start of gum grafting treatment. The thickness of the gingival and bone tissues affects the treatment outcomes, perhaps because of a difference in the amount of blood supply to the underlying bone and the susceptibility to resorption. I have found that most maxillary and almost all mandibular anterior tissue biotypes can be considered thin and susceptible to recession. When performing orthodontic tooth movement, restorative dentistry, implant treatment or periodontal care, the clinician must consider the possibility that recession can occur during or shortly after treatment. A periodontal consult to evaluate the need for gingival augmentation should be considered.
Minimally Invasive Treatment
The most minimally invasive treatment for recession and inadequate attached gingiva is the subepithelial connective tissue graft from the palate. This graft will provide a sustained increase in gingival thickness, keratinized tissue, and root coverage. No other treatment can make such a claim. The best graft material is the patient’s own tissue.
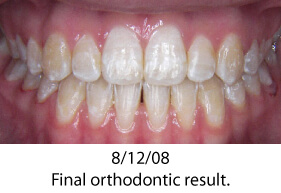
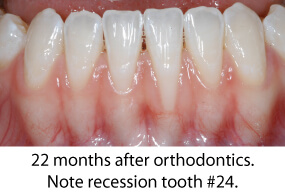
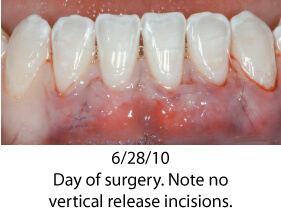
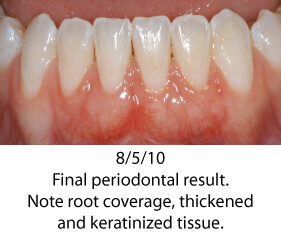
The photos below show a patient who had orthodontic care with an excellent final orthodontic result. Shortly after completion of orthodontics, severe recession occurred on tooth # 24. This case shows a very common finding; a thin periodontium where root form is visible through the gingival tissue. The gingival tissue was less than 1 mm in thickness so careful manipulation and suturing was necessary. Traditional techniques would require raising a flap with vertical release incisions over the adjacent teeth. Using a microsurgical approach was instrumental in treating this patient. The tissues were gently handled; sutured using 7-0/9-0 sutures and no flap was reflected. Wound healing was greatly enhanced by not raising a flap; circulation was minimally compromised and the forces from lip movement were significantly reduced. Each of these microsurgical steps leads to a finer surgical result, greater predictability and an easy post-operative recovery for the patient.