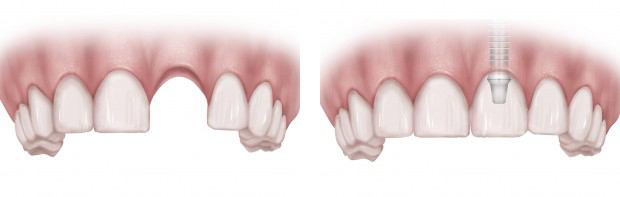
In the November issue of the Journal of Periodontology, an article entitled A 4-year evaluation of the peri-implant parameters of immediately loaded implants placed in fresh extraction sockets, authored by Roberto Crespi, considered the correction between the meaning of keratinized mucosa(KM) and the long-term maintenance of implants placed in fresh sockets and immediately loaded.
Methods: Twenty-nine patients requiring extractions of ≥2 teeth in the maxilla and mandible were selected. One-hundred thirty-two maxillary and 32 mandibular teeth, in the incisor, canine, and premolar regions, were extracted. Implants were positioned in fresh sockets and immediately loaded. Based on the amounts of KM, implants were categorized as follows: KM ≥2 mm (group A) and KM <2 mm (group B). Clinical parameters (probing depth, modified plaque index, modified bleeding index, and gingival index) and marginal bone levels were followed at 4 years after implant placement. Comparisons between group A and B values were performed by the Student two-tailed t-test.
Results: At the 4-year follow-up, a survival rate of 100% was reported for all implants. The mean values of group B were significantly higher (P <0.05) than group A for the following parameters: gingival index (group A, 0.67 – 0.09; group B, 1.01 – 0.11); modified plaque index (group A, 1.18 – 0.09; group B, 1.71 – 0.12); and modified bleeding index (group A, 0.35 – 0.05; group B, 0.78 – 0.05). Gingival recession was significantly elevated in group B. In both group A and group B, up to 60% of gingival recession occurred within the first 6 months. For mean bone loss values, statistically nonsignificant differences were reported between groups.
Conclusions: At a 4-year follow-up, the results suggested that the presence of mid-buccal KM is not a critical factor in the maintenance of interproximal bone level around fresh socket implants immediately loaded. Conversely, less width of KM is significantly associated with more gingival inflammation, more plaque accumulation, and more gingival recession.